Uniting to Save and Sustain Lives
We are seizing opportunities to expand global access to our medically essential product portfolio to support more patients through every point of their journey. Engage with us here for our Hillrom and Welch Allyn product and therapy portfolio.
We are seizing opportunities to expand global access to our medically essential product portfolio to support more patients through every point of their journey.
Featured Products
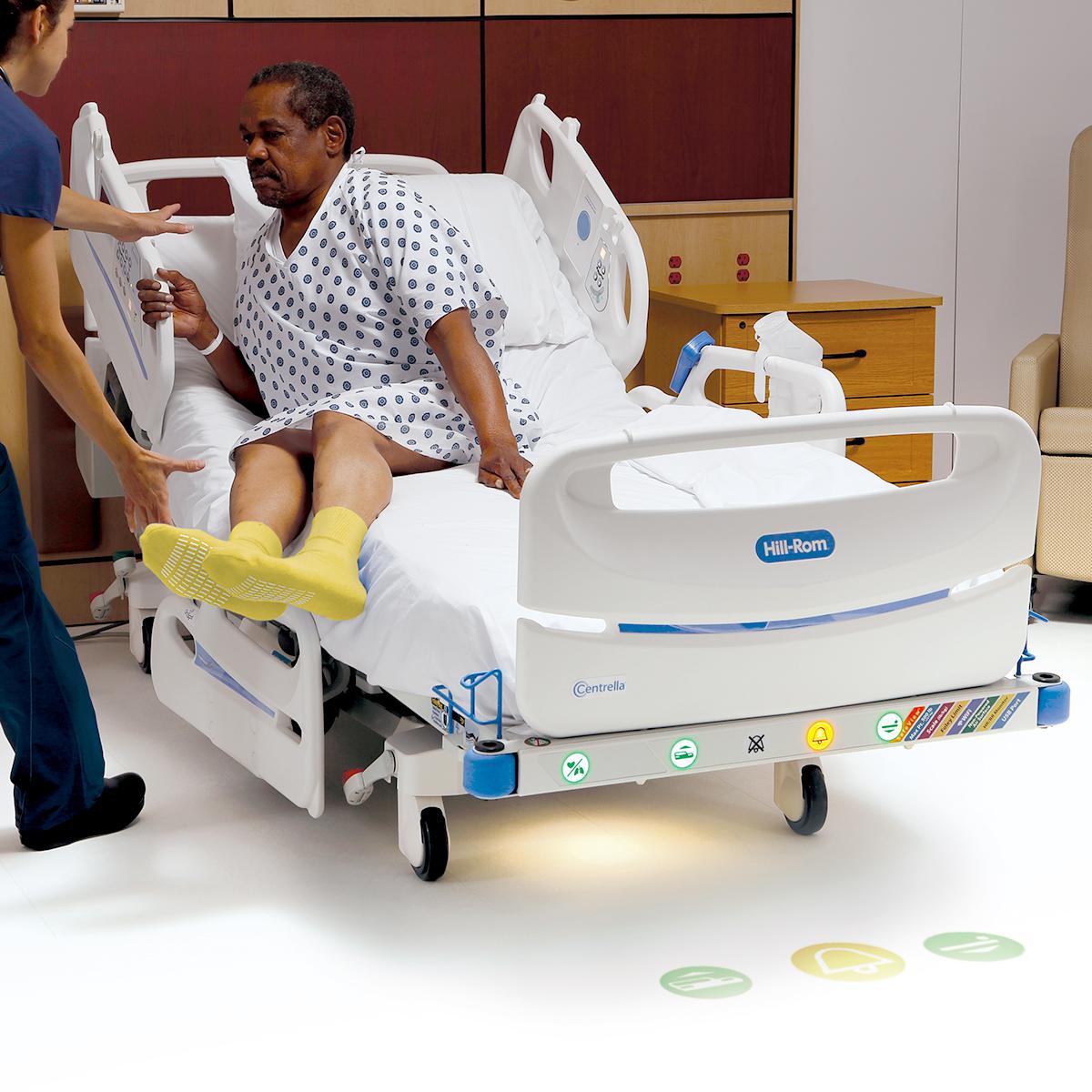
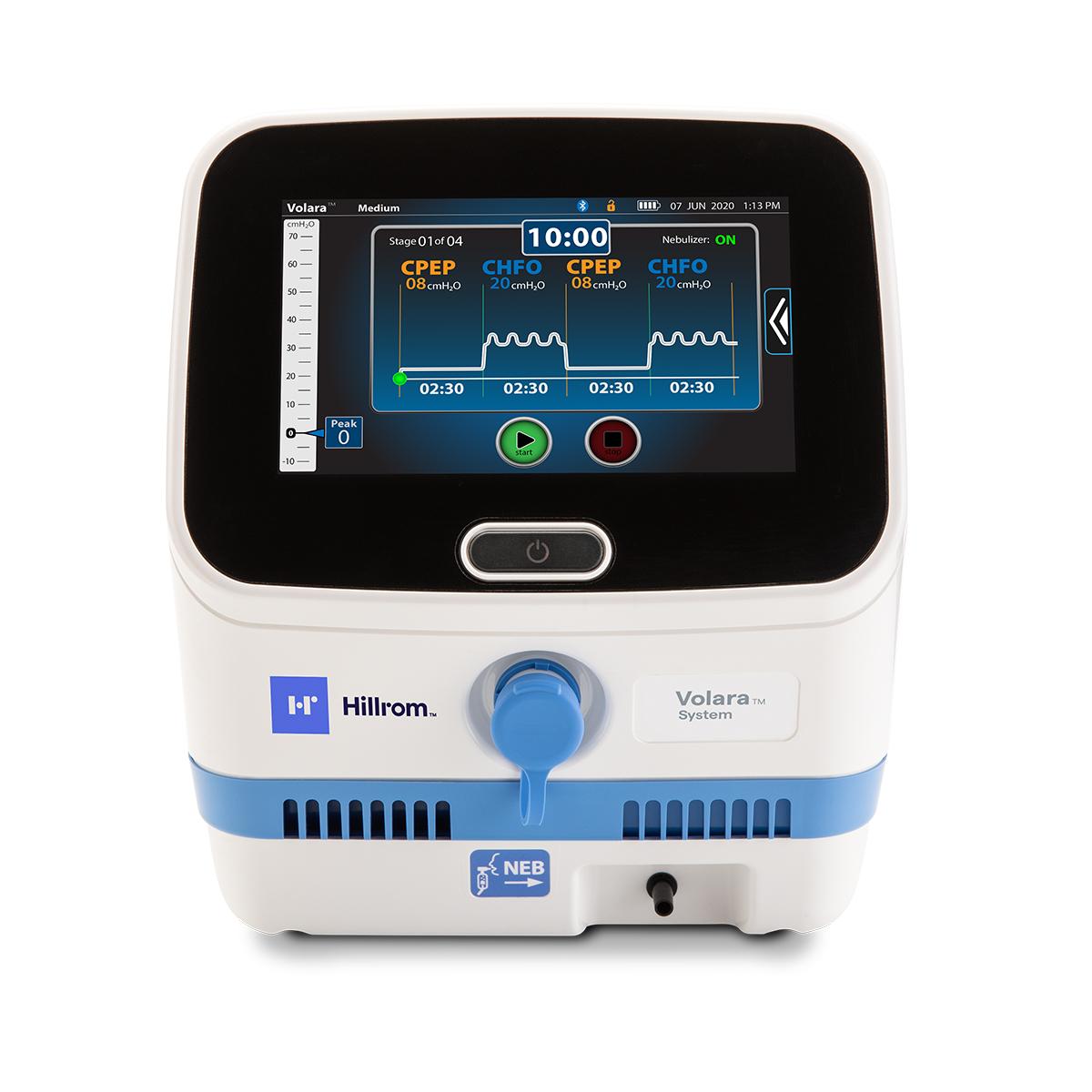
From next-generation smart beds to care communication apps, see how we're advancing connected care.
Check out our full product portfolio to see how we can help you enhance patient outcomes.
Get To Know Us

Put Your Passion for Helping Others to Work
Make a difference in the lives of others — and your own.

Where We Work
With more than 10,000 employees in over 100 countries, we offer global support that’s insightfully close.